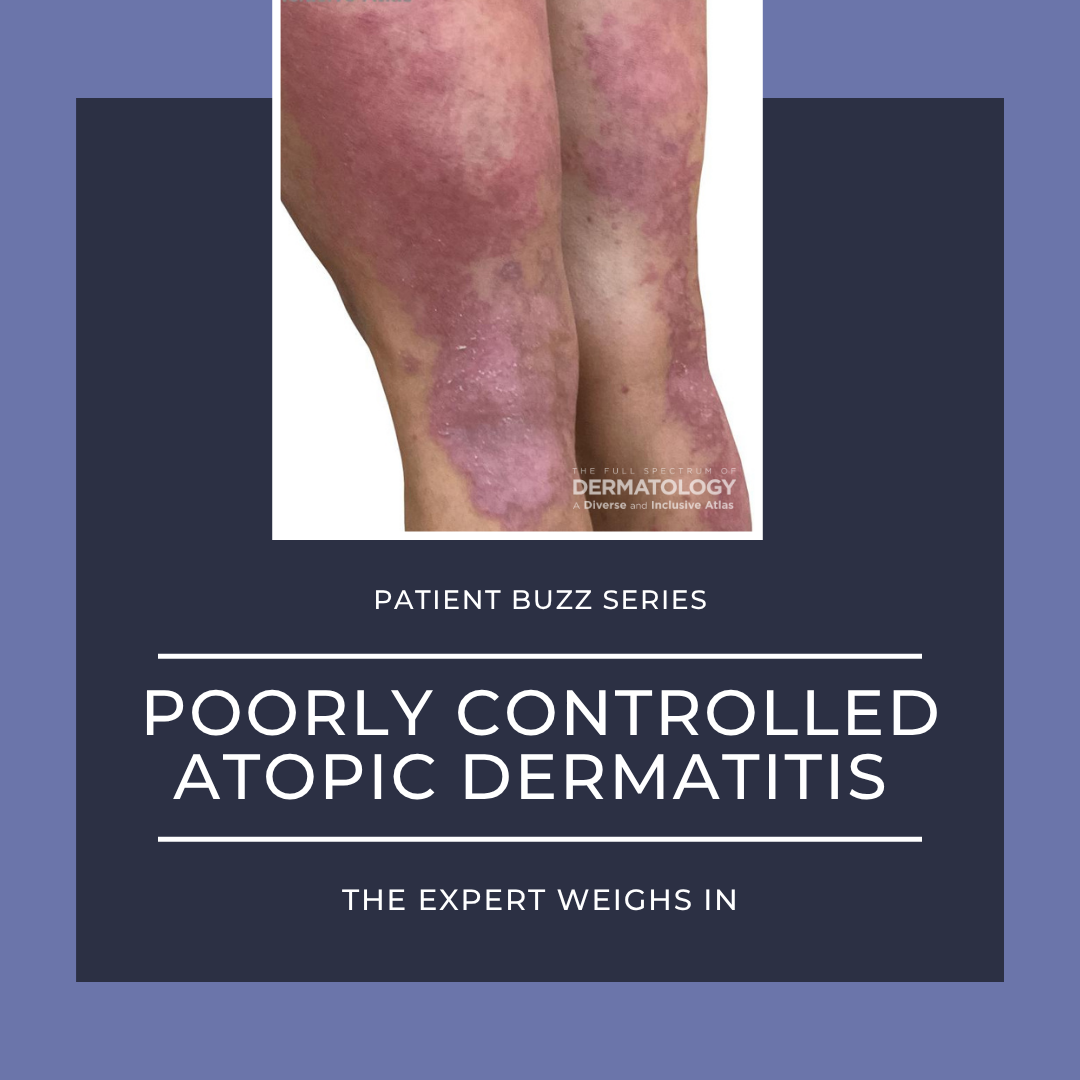
Atopic dermatitis (AD) that’s not fully under control was the subject of two Everyday Health articles: one on treatment “red flags” and another on insufficient care that’s accepted by patients as “good enough.” With so many factors contributing to AD flares, discerning when a treatment isn’t working or has stopped working can be a challenge for both patients and clinicians. Additionally, patients may have become so used to coping with flares that they settle for the status quo, unaware that newer treatments could provide significant improvements to their skin and quality of life.
For a practical take on AD treatment plans, I interviewed Peter Lio, MD, FAAD, clinical assistant professor of dermatology and pediatrics at Northwestern University Feinberg School of Medicine. Dr. Lio’s clinical work is exclusive to inflammatory skin conditions.
How often do you treat patients who are simply surviving with “good enough” AD care? What is your approach with these patients?
Honestly, it’s one of the most common situations I encounter. Patients have often been living with AD for so long that they’ve become inured to the itch, the sleep disruption, the skin that never quite clears. They come in not asking for better control; they’ve simply accepted their baseline as the ceiling. My approach starts with recalibrating expectations. I ask patients directly: “Do you wake up at night scratching? Do you avoid certain activities or clothes because of your skin?” I find that the Atopic Dermatitis Control Tool (ADCT) can really help capture this and help push back against patient resignation setting the clinical standard.
Since AD is multifactorial, how does a dermatology clinician know if a treatment is not working or has stopped working?
I find that the ADCT can really help here. Sometimes I find that if I start a visit with “How are you doing?” or “How are things going?”, the patient will smile and say: “Really good!” But once we go through the ADCT (it only takes 45 seconds!), they sometimes become very somber or even cry. People realize that they are not doing so well once they really think about it and ask the hard questions. The power of a structured tool is that it helps us do it the same way each time. But ultimately, the answer to the question is how the patient is doing. I often joke and say that we could do most of dermatology follow ups like this blindfolded: Even if they look bad, if they’re happy then I’m happy. And even if they look good, if they’re not happy then I’m not happy. So much of it is dynamic, temporarily changing, and very much how the patient is experiencing the illness. So little of it is what the skin might look like at the moment in time we happen to examine them, but that is counterintuitive for many.
When considering whether to rethink a treatment approach, what quality of life impacts do you consider? Are there certain impacts that you weigh more heavily than others?
Sleep disturbance is the one I weigh most heavily, because its downstream effects are so powerful: Mood, cognition, immune function, and family dynamics all suffer when a patient isn’t sleeping. Close behind that is work/school and social impact. A patient who has stopped going to the gym, withdrawn from social situations, or is missing work because of their skin is experiencing a level of disease burden that demands attention regardless of how their skin looks. I also ask specifically about anxiety and depression, since the bidirectional relationship between AD and mental health is well established and often undertreated. Quality of life is the outcome that matters most to the patient, and it should matter most to us.
How do you recommend dermatology clinicians work cooperatively with patients to develop and update treatment plans?
Shared decision-making is the foundation. Patients need to understand not just what we’re prescribing, but why, what realistic success looks like, and what the plan is if we don’t get there. I try to make the treatment roadmap explicit: Here is our first step, here is what we’re hoping to see by a certain timeframe, and here is what comes next if we need to escalate. I also try to invite patients into the conversation about their own priorities. Some patients want maximum clearance; others want to minimize medication burden. Both are legitimate goals, and the plan should reflect them. Revisiting the plan at every visit, even briefly, keeps it dynamic rather than passive. I made a mnemonic to help go through different medications.
Do you recommend patients track their symptoms, and if so, how?
Yes, and I try to frame it as empowering rather than burdensome. Tracking helps patients notice patterns they might otherwise miss: certain foods, stress triggers, environmental exposures, or seasonal shifts. I encourage simple, consistent tracking, whether that’s a dedicated app, a note on their phone, or even a paper journal. The key data points are itch severity, sleep quality, and any notable flares or triggers. Some patients find that photo documentation is especially useful for capturing what “bad” actually looked like, since memory is notoriously unreliable when it comes to chronic symptoms. Bringing that record to appointments also makes our conversations much more productive. The NEA has an app that can be helpful as does the Pierre Fabre Eczema Foundation.
What else should dermatology clinicians know about addressing poorly controlled AD?
Two things stand out. First, adherence and technique matter as much as the prescription itself. Many cases of “treatment failure” are really cases of undertreated skin, whether from concerns about the medications such as steroids, improper moisturizer application, or a regimen that simply doesn’t fit the patient’s lifestyle. Asking specifically about how and how often patients are using their treatments is always worthwhile. Second, the therapeutic landscape has changed dramatically, and patients with poorly controlled moderate-to-severe AD now have genuinely transformative options available. There is no reason a patient should continue to merely survive with their disease when biologic and JAK inhibitor therapies have redefined what remission can look like. If a patient remains poorly controlled on topicals, that is an indication to escalate, not to simply adjust expectations downward.
Did you enjoy this Patient Buzz expert commentary? You can find more here.