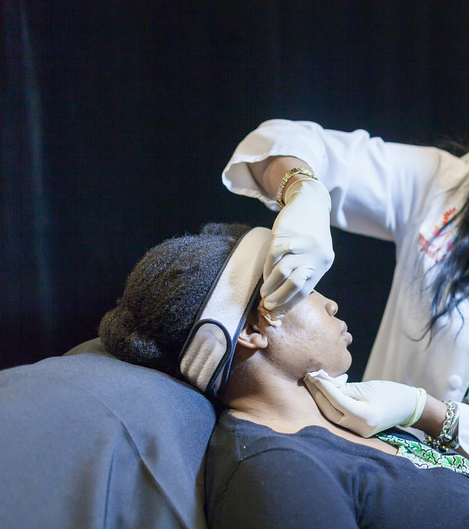
In Part II of our primer, we’ll focus on technique and aftercare. In case you missed it, view Part I of the series where we covered the basics of chemical peels.
Anesthesia
Choice of anesthetic will likely depend on the depth of the peel and patient preference. Superficial peels will likely cause only minor burning and stinging and usually require no anesthetic. Topical anesthetics can be considered for superficial to medium peels. Pharmacological sedation and/or nerve blocks should be considered for medium depth peels. Deep peels will likely require general anesthesia by an anesthesiologist who will also monitor the patient’s vital signs.
Preparing the Patient
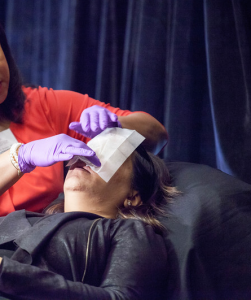 Prior to the procedure, the patient should be counseled about what to expect. They should be positioned comfortably at a 45-degree angle on the procedure table. The face should be cleansed and degreased with agents such as ethyl alcohol and/or acetone. A protective ointment such as petrolatum or zinc oxide paste should be applied to the lateral canthi, the bases of the nares and the oral commissures to prevent pooling in these areas.
Prior to the procedure, the patient should be counseled about what to expect. They should be positioned comfortably at a 45-degree angle on the procedure table. The face should be cleansed and degreased with agents such as ethyl alcohol and/or acetone. A protective ointment such as petrolatum or zinc oxide paste should be applied to the lateral canthi, the bases of the nares and the oral commissures to prevent pooling in these areas.
Technique
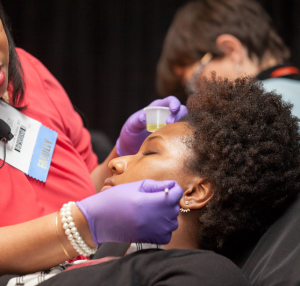 After pouring the peeling solution in a clean cup, care should be taken to remove any crystals in the solution to avoid uneven concentration. A general technique for all peels is to submerge a cotton tipped applicator or gauze pad in the peeling solution, removing any excess solution so as not to let it drip. Next, apply the peeling solution in even strokes starting with the forehead, then moving the cheeks, nose and chin. The clinician should take care not to overlap between strokes and to use a feathering technique. Careful technique should be used if treating areas such as the periocular skin, eyelids or lips, depositing controlled quantities of peeling solution. For solutions that produce frosting, a second or third pass may be needed to produce the desired result.
After pouring the peeling solution in a clean cup, care should be taken to remove any crystals in the solution to avoid uneven concentration. A general technique for all peels is to submerge a cotton tipped applicator or gauze pad in the peeling solution, removing any excess solution so as not to let it drip. Next, apply the peeling solution in even strokes starting with the forehead, then moving the cheeks, nose and chin. The clinician should take care not to overlap between strokes and to use a feathering technique. Careful technique should be used if treating areas such as the periocular skin, eyelids or lips, depositing controlled quantities of peeling solution. For solutions that produce frosting, a second or third pass may be needed to produce the desired result.
Aftercare
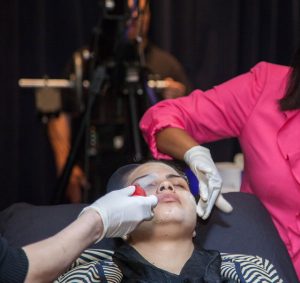 General aftercare for any peeling procedure should include diligent sun protection with sunscreen and sun avoidance. Patients should use a gentle cleanser on a daily basis followed by a bland moisturizer. It is of utmost importance the patient avoids picking at or peeling any flaking skin as this may increase their risk of adverse outcomes. They can resume topical retinoids and/or hydroquinone after re-epithelization in order to preserve/augment the effect of their peels. Written information should be provided to the patient about all of the above. It is also a good idea to have a follow up appointment in place soon after the peel in order to check on the patient and reassure them that their results are coming along as planned.
General aftercare for any peeling procedure should include diligent sun protection with sunscreen and sun avoidance. Patients should use a gentle cleanser on a daily basis followed by a bland moisturizer. It is of utmost importance the patient avoids picking at or peeling any flaking skin as this may increase their risk of adverse outcomes. They can resume topical retinoids and/or hydroquinone after re-epithelization in order to preserve/augment the effect of their peels. Written information should be provided to the patient about all of the above. It is also a good idea to have a follow up appointment in place soon after the peel in order to check on the patient and reassure them that their results are coming along as planned.
Did you enjoy this post? Find other articles on Aesthetic Derm Topics by clicking here.