Let us set the tone. Dr. Vivian Shi makes it clear. The goal is not to remove or replace prescription medications completely and “go all-natural”. What we are trying to do is provide evidence-based data to complement conventional therapy. We want what people are doing, to work. The goal is to empower our patients to strategically find a diet toolbox that works for their particular skin type and skin disease. “This is what I do. Integrative dermatology.”
So, who is getting acne? Dr. Shi points out that the prevalence of acne is higher in the “Westernized” population.” So, what is different about what we eat?
-
- High in cow’s milk and milk products, which come with hormonal effect
- High carbohydrate, protein, and fat contents
- Higher glycemic load
All of these components in the Westernized diet could contribute to acne. So how? How does the grease and sugar that a person eats make it to their skin? Whether it is milk, sweets, or fat, these enter the bloodstream as free sugar (glucose) and stimulates the release of hormones (insulin, insulin-like growth factor-1) within the body. These hormones cause a cascade resulting in skin cells to be more sensitive and receptive to the hormonal influence in the diet. So, what does this mean? A Western diet may cause:
-
- Follicular occlusion by:
-
-
- Increased skin cells building up in the hair follicle (pilosebaceous unit)
- Abnormal shedding of hair follicle cells (desquamation)
- Increased oil (sebum) production
-
-
- Increased bacterial growth
- Increased inflammation
How about the good and bad in individual foods?
What could be bad?
Things to have less of in a diet:
-
- High glycemic index foods: Simple carbohydrates that break down quickly and cause spikes of free sugar.
- Dairy
- Red Meat
Protein: Whey vs Casein vs other? Whey protein is rapidly digested causing a surge of protein. It is important to avoid the surge in protein, just like avoiding a surge of free sugar in the blood. Among the dairy proteins, casein is more slowly digested and has extended release into the blood.
Some skin-friendly alternatives to whey protein powder include hemp seed, brown rice, pea, soy isolate, egg white, and plant protein blends. Remember the benefit of the complete amino acid pairs. Rice and beans provide a complete set of proteins that the body needs.¹ Dr. Shi personally prefers the soy isolate protein not only because of the taste but also because in soy isolate the estrogen-like hormone components are preferentially removed, thus, negating any concerns that people may have with soy and estrogen. Brown rice protein is high in iron and good for those with anemia, like menstruating women. Egg white protein has high bioavailability and is nearly completely absorbed by the body.
Milk: So, what about milk? Milk has a lot of hormonal mediators which can worsen acne. Some are “spiked” with anabolic steroids and growth factors such as progesterone. These are going to increase oil production (sebogenesis). Although lower in fat, skim milk is the most incriminated when it comes to acne, more so than whole milk. Although we do not know how entirely, due to extra processing, skim milk may have less estrogen which would normally balance out the acne forming progesterone.
What could be good?
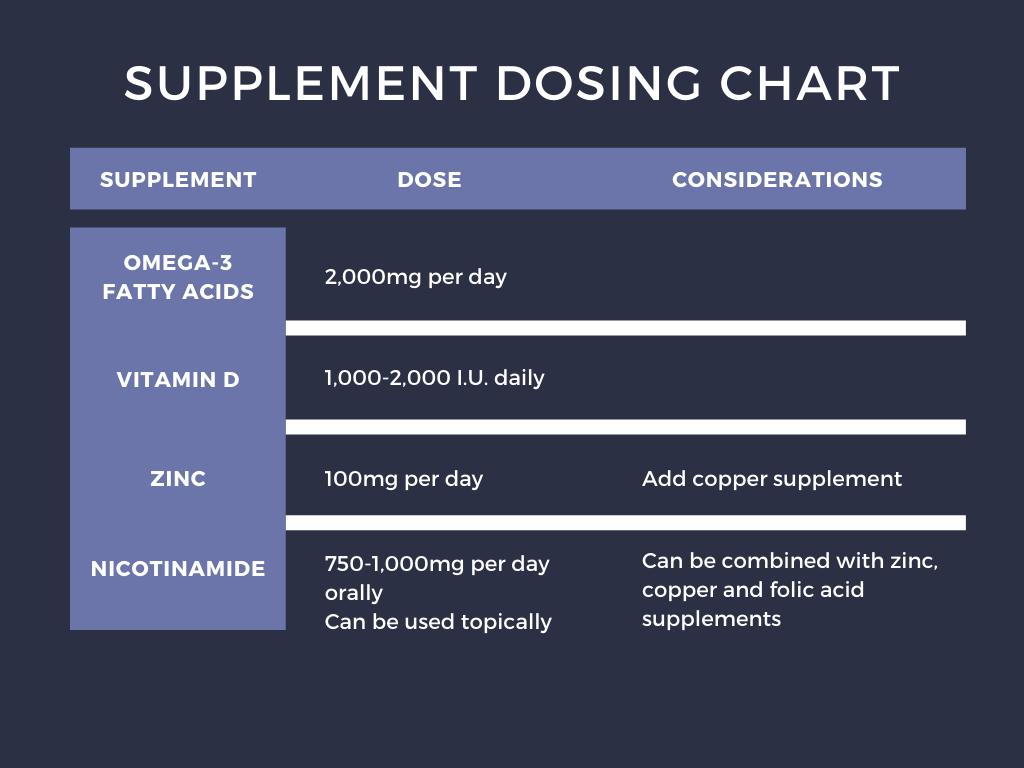
Omege-3 fatty acids (2,000mg) vs borage seed oil (gamma-linoleic acid 400 mg) vs normal diet (control):
In patients with mild to moderate acne, diets supplementing with omega-3 and borage seed oil showed less inflammatory and non-inflammatory lesions as well as decreased overall acne severity.²
Vitamin D: Patients with acne are more likely to have acne than those who do not (50% vs 23%). In fact, lower levels of vitamin D can correlate with more inflammatory acne. In patients with inflammatory acne, vitamin D3 (1000 I.U. daily for at least 2 months) may help.
Zinc (30-200mg per day): Zinc may help the liver to release vitamin A, which is our most effective tool for combating acne. Patients with lower zinc have been shown to have more severe acne. Dr. Shi’s preferred dosing falls in the middle, 90-100mg per day. Zinc can cause nausea, vomiting, or inflammation of the esophagus (esophagitis). Zinc gluconate is the easiest to find over the counter while zinc picolinate is the best tolerated and least irritating. Also, zinc competes with copper for intestinal absorption, and long term high dose zinc supplementation could cause copper deficiency. If taking zinc long term, a person must take copper supplements at a 10:1 zinc to copper ratio. So, for 100mg zinc per day, 10mg of copper should be taken as well.
Oral Nicotinamide (vitamin B3): Nicotinamide can lower the production and affect inflammatory markers (IL-8)³ and when taken orally can reduce acne. This can be combined with oral zinc, copper, and folic acid to have synergistic effects. A study has shown that this combination of supplementation was similar to that seen in patients taking oral antibiotics for their acne.4
Topical 4% Nicotinamide: Topical nicotinamide had a similar improvement as compared to 1% clindamycin gel. Nicotinamide performed better for patients with oily skin, whereas clindamycin was better with non-oily skin. It is worth noting that the formulation of these topical products and medications could make a difference in their effect on acne.
Although we have been able to draw some conclusions based on available research, there remains to be a lot of unknowns on nutrition and acne, including chocolate, caffeine, and alcohol. If looking for a dietary program already in place to get started, the paleolithic and Mediterranean diets are generally a good starting point.
For more detailed information on how nutrition is affecting inflammation in the skin, please see Dr. Shi’s paper on the topic.5
References:
-
- FDA, interactive nutrition fact labels. Access data. Protein. March, 2020. Accessed Aug, 5th 2020. https://www.accessdata.fda.gov/scripts/InteractiveNutritionFactsLabel/assets/InteractiveNFL_Protein_March2020.pdf
- Jung JY, Kwon HH, Hong JS, et al. Effect of dietary supplementation with omega-3 fatty acid and gamma-linolenic acid on acne vulgaris: a randomised, double-blind, controlled trial. Acta Derm Venereol. 2014;94(5):521-525. doi:10.2340/00015555-1802
- Grange PA, Raingeaud J, Calvez V, Dupin N. Nicotinamide inhibits Propionibacterium acnes-induced IL-8 production in keratinocytes through the NF-kappaB and MAPK pathways. J Dermatol Sci. 2009;56(2):106-112. doi:10.1016/j.jdermsci.2009.08.001
- Niren NM, Torok HM. The Nicomide Improvement in Clinical Outcomes Study (NICOS): results of an 8-week trial. Cutis. 2006;77(1 Suppl):17-28.
- Maarouf M, Platto JF, Shi VY. The role of nutrition in inflammatory pilosebaceous disorders: Implication of the skin-gut axis. Australas J Dermatol. 2019;60(2):e90-e98. doi:10.1111/ajd.12909

