What has been your most challenging condition to treat? I’d be willing to bet that hidradenitis suppurativa (HS) would be at least one (if not the top) answer. The pain/suffering that HS patients endure brings me to tears sometimes. Do you share this sentiment? If so, I hope to empower you with practical pearls from Dr. Adam Friedman, Professor and Interim Chair of Dermatology, Residency Program Director, Director of Translational Research, and Director of the Supportive Oncodermatology Clinic in the Department of Dermatology at The George Washington University School of Medicine & Health Sciences.
Pathophysiology
Like many other chronic inflammatory disorders, HS pathophysiology is multifactorial. There are modifiable factors including smoking, obesity, mechanical, and environmental factors. But genetics is a huge component. A third of HS patients have a first degree relative with the disease! Hormones also play a role, and there may also be an infectious component. All these factors lead to the dysregulation of the innate immune system, causing chronic (not autoimmune) inflammation that becomes difficult to control.
Is There A Gap In Clinical Care?
The answer is a resounding yes! HS is often not recognized, and diagnosis is delayed for an average of 6-10 years. This means– by the time the patient presents, the disease is already progressed, which will have resulted in more pain, impaired function, wasted time and money, and frustration. Why the delay? With a long list of mimickers– including acne, cellulitis, inflamed cyst, lymphadenopathy, perirectal abscess, pilonidal cyst, Crohn’s disease, lymphogranuloma venereum, and infections– HS unfortunately is a challenging diagnosis, if we are not thinking about it.
How Do You Diagnose HS?
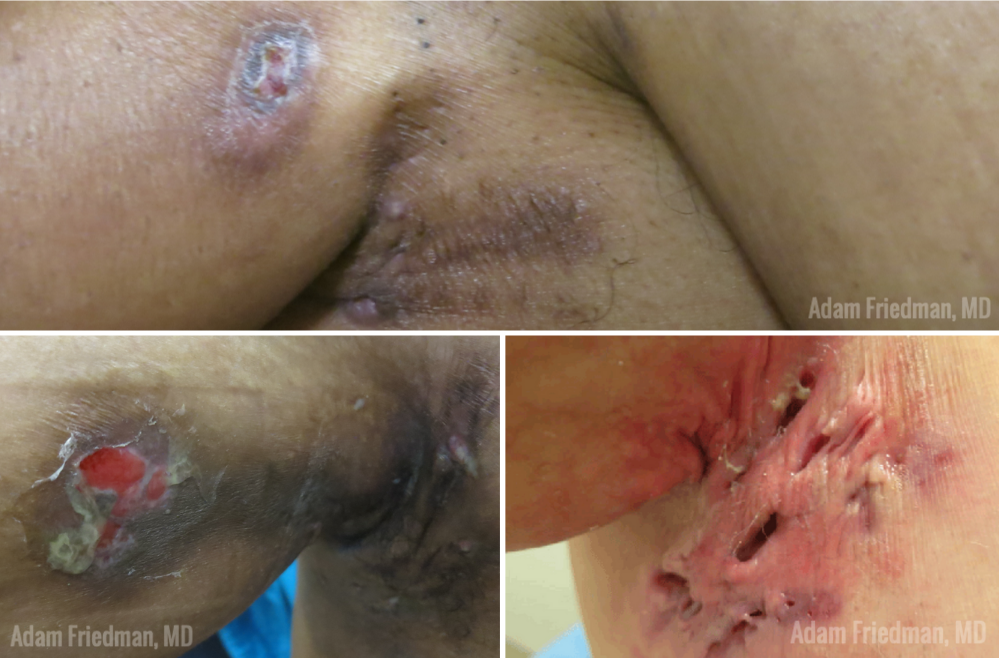
Three criteria need to be met for diagnosis: 1) having typical lesions (painful deep-seated nodules with possibly abscesses, draining sinuses, bridged scars, “tombstone comedone”), 2) typical location, and 3) chronicity (>6 months) and recurrences. Perianal/genital involvement is more common in men, while women more often have inframammary and axillae lesions.
Typical lesions would be painful, deep-seated, abscesses-like structures that, over time, turn into scarred sinus tracts in intertriginous areas. When you see a painful red nodule in these areas, the natural instinct may be to call it an infection (and it may be). But, please ask about how long the same lesion has been present, in the same location, look for scarring and draining sinuses—and maintain a suspicion for HS.
Treatment
Pop quiz: how many drugs are FDA-approved for HS? Think about everything you’ve prescribed for your HS patients. Maybe…ten? Nope. Five? Try again. The answer is one! That’s right– one FDA-approved medication for this terribly debilitating disease. (Which one is it? We will discuss— keep reading!)
First, counsel patients regarding the chronic nature of this disease and set realistic goals together. Education regarding modifiable factors is very important.
- Mostly importantly, stop smoking! A recent study showed that response to first-line medical therapy was lower in smokers vs. non-smokers.
- Certain medications, including androgenic medications, progestins (e.g., Mirena IUD, Depot medroxyprogesterone acetate), and lithium should be avoided.
- Reduce stimuli that lead to pore rupture: reduce friction/heat/sweating, wear loose clothing, use tampons instead of pads, no picking or squeezing
- Weight reduction: low glycemic and low dairy diet
In many conditions, we apply the “step therapy” approach, where we start with one medication and add or move onto another one if it fails. Well, HS should not be one of them. We need to address the different aspects of HS concurrently, and hit them hard. Here are some options in our toolbox.
- Intralesional kenalog (ILK) – the quick fix
- Great for acute flares!
- ILK (10mg/ml injections in one study led to pain reduction in 1 day and signs of inflammation 7 days later)
- Antibiotics (off-label) are used for their anti-inflammatory effects and to “normalize the skin flora” by decreasing pathologic bacteria
- Clindamycin/rifampin 300mg BID has the best data! So start here.
- Interestingly, a recent study (n=30, 8 weeks) showed that clindamycin alone (at 150mg every 8 hours) was just as effective, if not a little better, compared to the combo therapy. That’s nice to know, for those who would rather skip the rifampin! This is great for patients on oral contraceptives, which are metabolized by rifampin (=cyp inducer) and rendered ineffective.
- Surprisingly, tetracyclines have limited data. In one clinical trial, efficacy was equivalent to topical clindamycin at 16 weeks.
- Other possible therapies:
- Rifampin 10mg/kg daily, moxifloxacin 400mg daily, and metronidazole 500mg TID added for 6 weeks
- Dapsone can be a relatively safe option that has shown efficacy as well.
- Is antibiotic resistance is real? Oh yes, and with some convincing data.
- Topical clindamycin: Antimicrobial resistance against clindamycin-resistant Staph aureus was 63% vs. 17% (p=0.03) compared to non-users
- Oral trimethoprim/sulfamethoxazole (TMP-SMX): TMP-SMX-resistant Proteus species was 88% vs. 0% (p<0.001) compared to non-users.
- No resistance reported (yet?) with tetracyclines and oral clindamycin, but only time will tell.
- Combining an oral antibiotic with a topical antimicrobial doesn’t seem to make a huge difference on resistance, except for cephalosporins—will likely reduce development of chronic yeast (in a small study).
- Anti-hormonal treatment– Don’t be shy. Give it a try!
- Women: Spironolactone 50-100mg twice daily. (Dr. Friedman says almost all his female HS patients are on spironolactone and responding well!)
- Men: Finasteride 1-5mg daily
- Retinoids (acitretin and isotretinoin). Take-home message here: high dose is good for early (stage 1) disease.
- An early “Dr. Steven Cohen” high-dose therapy (200-220mg/kg) may be able to “reset the clock,” potentially changing the anatomy and preventing progression. However, once progression has begun, efficacy is much less reliable.
- Biologics—a game changer. This is for severe/extensive disease and can be life-altering (albeit not a cure).
- And yes, adalimumab is the only FDA-approved medication for the treatment of HS!
- In one study, response rates varied from 42 to 59% in achieving at least 50% reduction in total inflammatory lesions, no new lesions, no new sinus tracts.
- What about long-term data? A 3-year follow-up study showed that efficacy was maintained in 60% of the patients.
- Current data on IL-17 inhibitors
- Secukinumab has shown efficacy in some case reports. Currently, there is a clinical trial evaluating efficacy of secukinumab. So, stay tuned!
- While data are not robust, ustekinumab and apremilast may work. They can certainly be considered if all options have been exhausted.
- And yes, adalimumab is the only FDA-approved medication for the treatment of HS!
Other Treatment Considerations
What about supplements? Zinc deficiency is more prevalent in HS patients, so supplementation is recommended. Zinc 50mg with 2mg of copper amino acid complex is recommended. Vitamin C can be recommended at 1000mg BID.
Lastly, let us not forget about pain control. Combination of acetaminophen 1000mg and ibuprofen 400mg (at the same time) every 4 hours up to 4 doses is a nice go-to. Gabapentin can also be helpful (most patients responding at doses of 900 to 1800mg daily). But, watch out: tolerance occurs rather quickly, so be proactive about discussing accidental overdose and the FDA warning of increased suicidal acts or violent deaths.
Final Pointers
Don’t climb up the ladder in choosing your therapy. Rather, address multiple factors all at once. Remember that combo is king (recurrent theme), and recruit your army of referrals (plastic surgeon, general surgeon, psychologist, and psychiatrist…) who can also help optimize your care for this debilitating condition.
And finally, let us not lose hope. For these patients, we may be the only advocate. It’s well worth the fight!
This information was presented by Dr. Adam Friedman at the 16th Annual ODAC Dermatology, Aesthetics and Surgical Conference held January 18th-21st, 2019 in Orlando, FL. The above highlights from his lecture were written and compiled by Dr. InYoung Kim, one of the 5 residents selected to participate in the Sun Resident Career Mentorship Program (a program supported by an educational grant from Sun Pharmaceutical Industries, Inc.). Dr. Kim was paired with Dr. Friedman as her mentor.
All images courtesy of Dr. Adam Friedman.