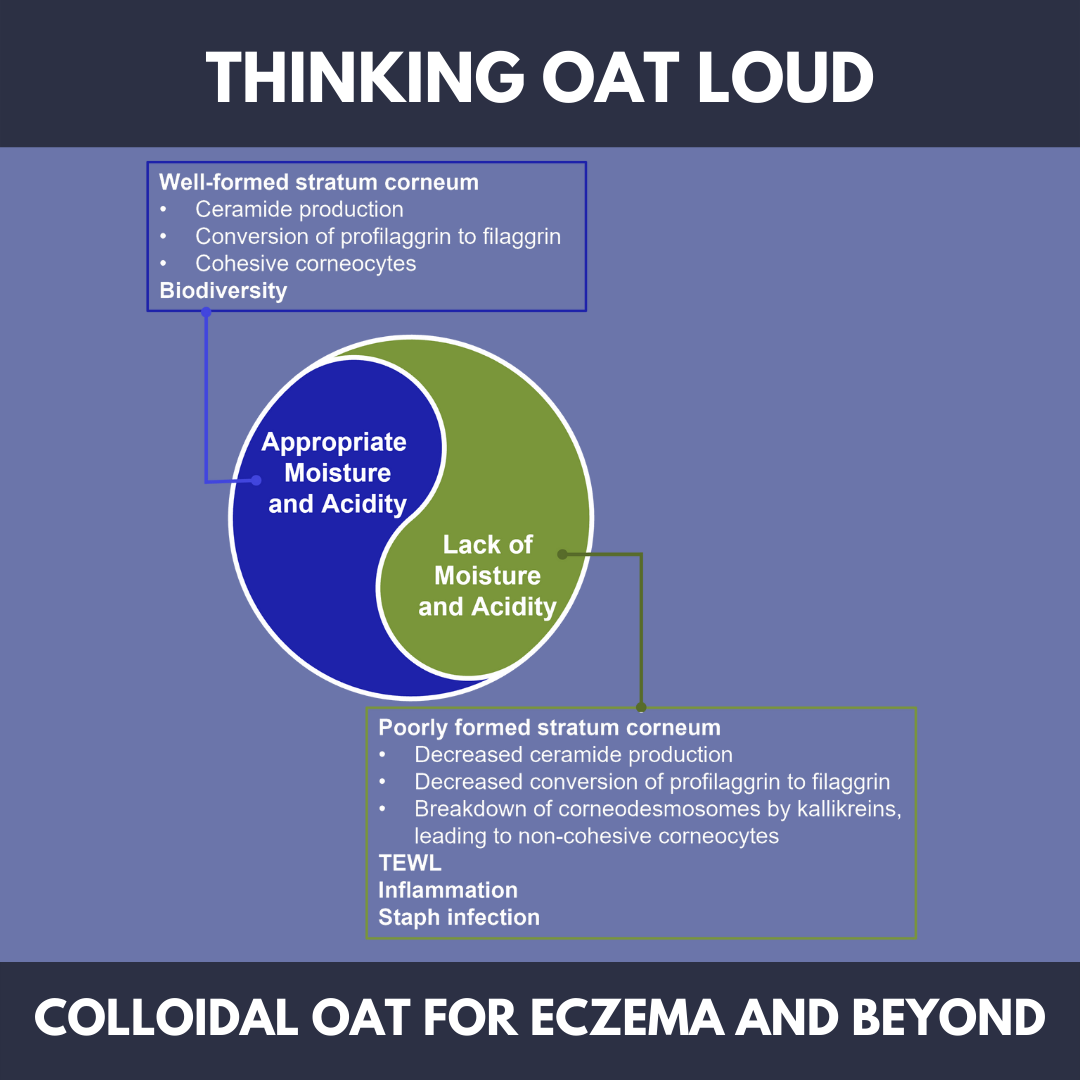
Atopic Dermatitis Pathogenesis
Atopic dermatitis (AD) is a chronic inflammatory skin disease for which common symptoms are rash, itch, dryness, and redness. AD is a perfect example of what happens when skin barrier homeostasis is not maintained. In AD, the lipids that comprise the skin barrier are reduced in chain length compared with healthy skin, resulting in poor barrier function and increased water loss. The changes in skin barrier lipid properties also correlated with the severity of AD.1 The two most important factors affecting skin barrier homeostasis, and by extension, skin health, are moisture and acidity. For example, acidity is important for maintaining biodiversity in the microbiota naturally present in the skin. In healthy skin, Staphylococcus aureus is one of many bacterial species competing for resources. A higher skin pH allows S aureus to flourish, while other microbiota die out. At baseline, patients with AD have a more basic skin pH level compared with non-AD patients, so it’s no surprise that staph infections are more common in patients with AD. Additionally, when skin pH increases, ceramide production decreases, conversion of profilaggrin into filaggrin is stunted, and kallikreins break down the corneodesmosomes that hold the corneocytes of the stratum corneum together. This results in a poorly formed stratum corneum and causes subsequent transepidermal water loss (TEWL). TEWL results in “leaky skin,” which is more susceptible to infection and disrupts healthy cells replacing dysfunctional cells.
Beyond environmental factors that affect healthy skin (eg, moisture and acidity), genetics and age predispose patients to AD. Variations in the gene that produces filaggrin are relatively common in patients with AD, resulting in a lack of biologically active filaggrin peptides.1 Additionally, with increased age, skin pH can also increase. Clinically, AD can manifest as dry skin (xerosis), itchy skin (pruritis), and/or cracked skin.
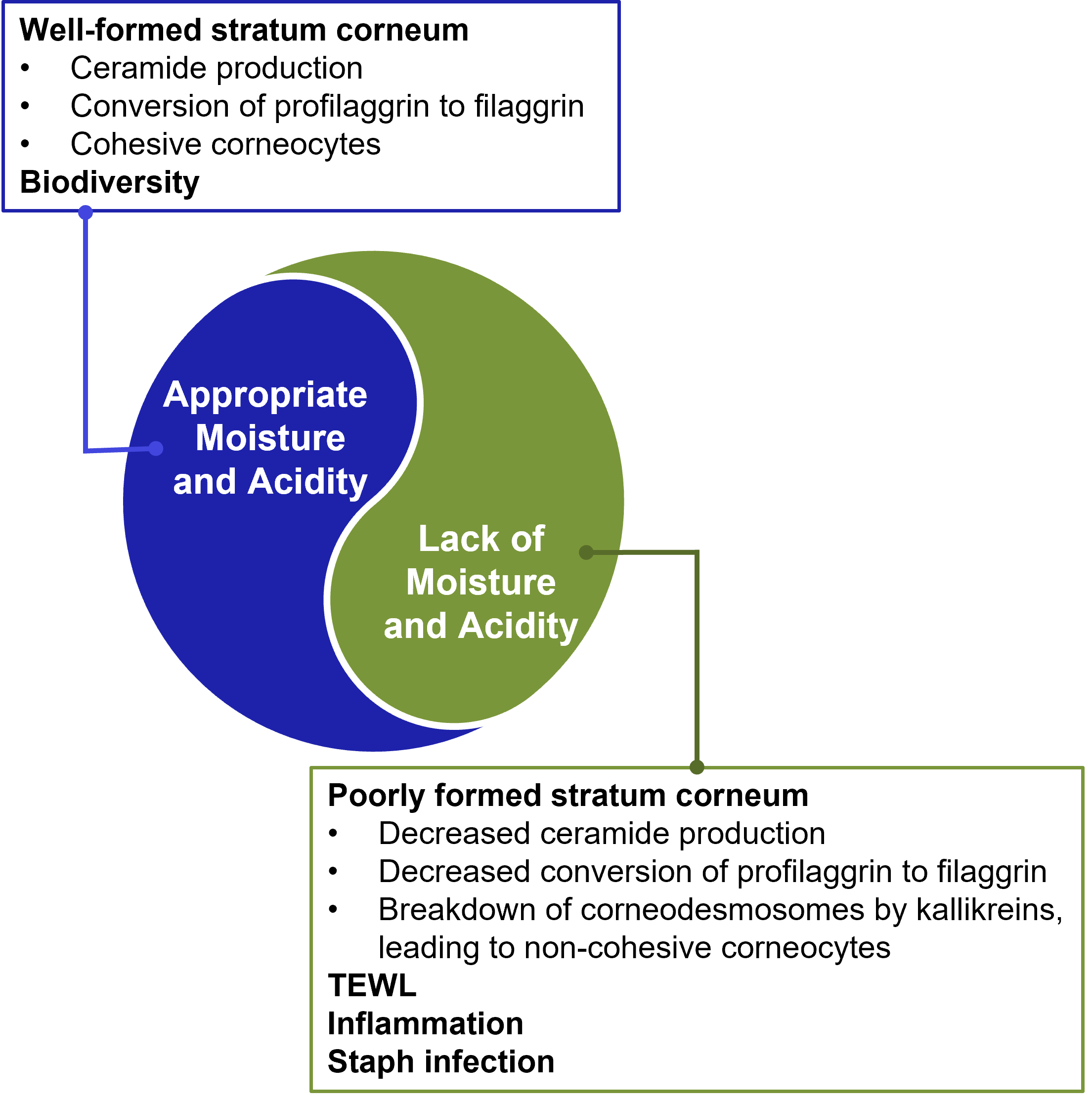
In addition to barrier dysfunction, atopic skin is characterized by immune dysregulation. S aureus can increase the body’s inflammatory response, leading to T2 inflammation, which can negatively impact proper production of the stratum corneum. Atopic skin that shows no signs of infection is still histologically abnormal.
Treating AD
The foundational treatment for over-dried, over heated skin is consistent, gentle skin care. Applying moisturizer to damp skin should be part of your daily routine, like brushing your teeth. The next step in the treatment ladder is topical or oral medication to supplement the daily skin care regimen. Finally, in some cases, systemic therapy for AD is required.

Colloidal Oat: The T-OAT-al Package
Oatmeal has been used as a skin care ingredient since 2000 BC in ancient Egypt, where whole oats were used in soothing baths. Colloidal oat has been the subject of dedicated skin care research starting in the 1950s. After > 30 clinical studies comprised of over 3000 patients including conditions associated with a compromised skin barrier, colloidal oat is now recognized as a skin protectant by Health Canada and the US FDA, which acknowledged it as the only natural ingredient that can claim to protect and relieve symptoms of eczema. Colloidal oat contains avenanthramides, which are polyphenols that confer anti-inflammatory and antioxidant properties.
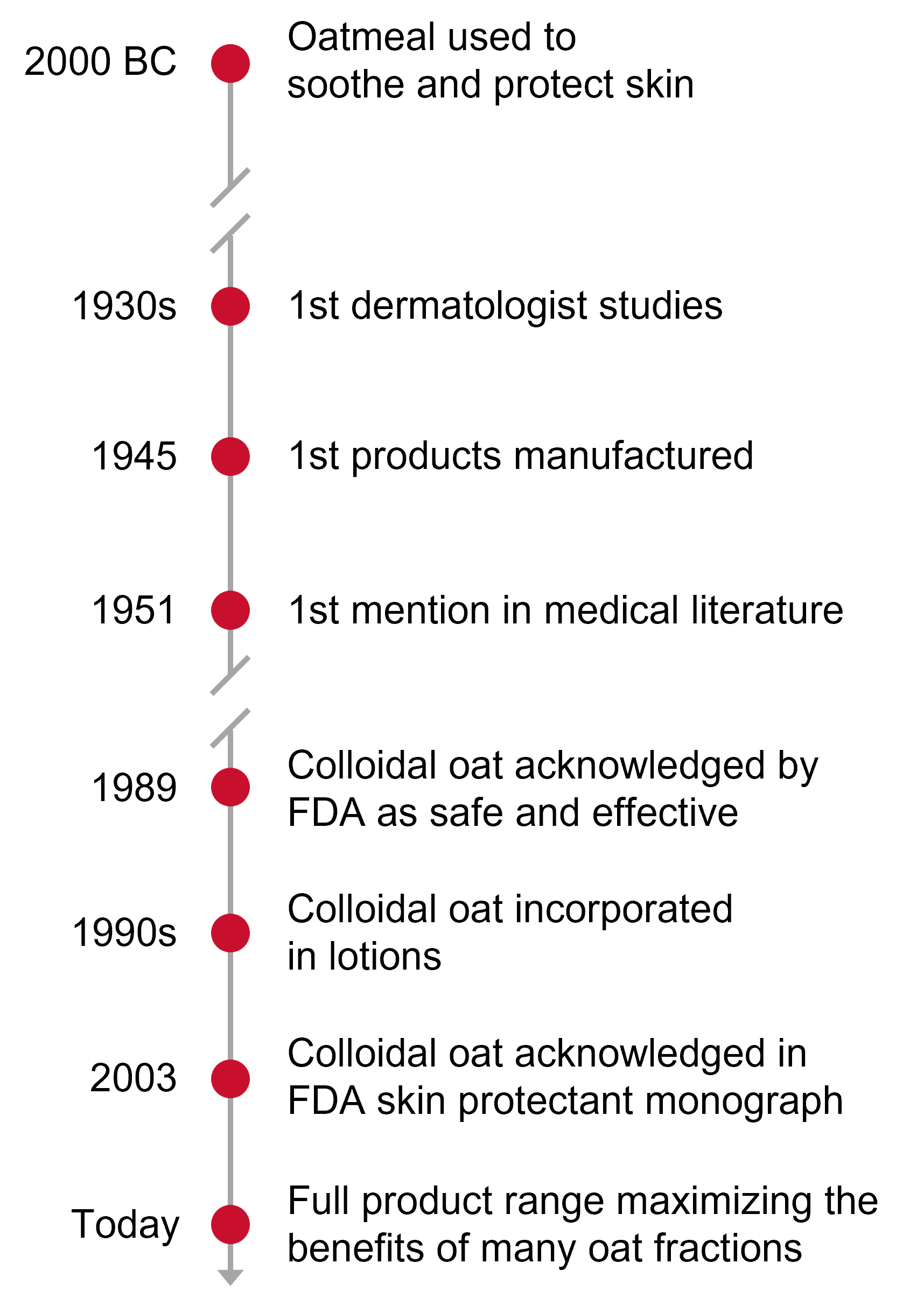
Preclinical data in inflamed human keratinocytes has shown that avenanthramides reduced cytokine production, and a clinical study demonstrated the ability of topically applied avenanthramides to relieve the symptoms of ultraviolet light-induced erythema (reddening of the skin), including itch.2
In a clinical study of patients with xerosis and pruritis, the oat-containing lotion was tested versus its vehicle which contained some humectants including glycerin. The oat-containing lotion (including oat extract and oat oil) reduced overall skin dryness, scaling, and patient-assessed itch intensity, duration, and frequency.3 Moreover, patients preferred the appearance and texture of the oat-containing lotion.
While commercial ceramide products replace the naturally produced ceramides whose production is decreased in AD, oat oil (a component of colloidal oat) has been shown to stimulate natural production of ceramides in vitro. Colloidal oat also increases the diversity of commensal skin bacteria, which can decrease the prevalence of S aureus in patients with AD.

Beyond Eczema
Oat-containing lotion is being investigated for use in the non-AD patient population as well. In a study of diabetic patients with lower leg dryness, erythema, fissuring, scaling, and tactile roughness improved as early as 1 week into twice-daily use of oatmeal-based moisturizing lotion.4 In patients with mild psoriasis, once-daily, full-body oatmeal lotion use (with a focus on dry patches) led to improvements in perceived dryness, roughness, desquamation, discomfort, itch, and redness.5
Anticancer therapies, including immunotherapies targeting transforming growth factor-β and epidermal growth factor receptor (EGFR) as well as radiation therapy, often cause adverse events affecting the skin (eg, skin eruptions due to EGFR inhibition or radiation‑induced fissures). EGFR inhibition can cause skin barrier disruption within a matter of hours. Oat-containing lotions have been used to manage adverse events associated with anticancer treatments, including xerosis and pruritis.6
Summary
In conclusion, AD is characterized by moisture loss and higher skin pH, which lead to disruption of the skin barrier and immune dysregulation. Gentle and consistent skin care remains the first line of defense in combating AD, which can be supplemented with topical/oral medications and systemic therapies in more severe cases. Oat-containing lotions can be used to alleviate the symptoms of AD, as well as address the underlying pathophysiological mechanisms. In addition to its use in AD, colloidal oat has been investigated as a treatment for psoriasis, skin issues associated with diabetes, and adverse events resulting from anticancer therapies. An Instagram Live post featuring a discussion of colloidal oat between Dr Adam Friedman and Dr Blair Allais can be viewed here.
Products to Consider

Disclosures
Adam Friedman, MD
-
- Consulting/Ad board: Loreal, La Roche Posay, Galderma, Aveeno, Microcures, Pfizer, Novartis, Menlo, Lilly, Mino labs, Dermira, Zylo Therapeutics, Hoth therapeutics, Regeneron, Sanofi, Abbvie, Insed, Brickell Biotech, Incyte, UCB
- Speaker: Regeneron/Sanofi, Abbvie, Janssen, Brickell, Incyte
- Grants: Pfizer, Dermatology Foundation, Incyte, Galderma
Blair Allais, MD
-
- No disclosures
References
-
- Kezic S, Novak N, Jakasa I, et al. Skin barrier in atopic dermatitis. Front Biosci (Landmark Ed). 2014;19:542–556.
- Fowler JF, Jr. Colloidal oatmeal formulations and the treatment of atopic dermatitis. J Drugs Dermatol. 2014;13(10):1180–1183; quiz 1184–1185.
- Kalaaji AN, Wallo W. A randomized controlled clinical study to evaluate the effectiveness of an active moisturizing lotion with colloidal oatmeal skin protectant versus its vehicle for the relief of xerosis. J Drugs Dermatol. 2014;13(10):1265–1268.
- Nebus J, Wallo W. Safety and tolerance of skin protectant lotions with oat in patients with diabetes. Paper presented at: American Academy of Dermatology Annual Meeting 2008.
- Nollent V, Nebus J, Lisante TA. Tolerance and subject satisfaction of an over the counter colloidal oatmeal (Avena sativa) lotion in patients with psoriasis and sensitive skin. Paper presented at: American Academy of Dermatology Annual Meeting 2020.
- Lacouture ME, Cotliar J, Mitchell EP. Clinical management of EGFRI dermatologic toxicities: US perspective. Oncology (Williston Park). 2007;21(11 Suppl 5):17–21.
This article is brought to you by Next Steps in Derm in partnership with Johnson & Johnson Consumer Health.
Did you enjoy this article? You can find more on our OTC Resource Center.