Dear Next Steps Readers,
My name is Misty Eleryan, and I’m so glad to be one of the Content Contributors for Next Steps in Derm. In the upcoming weeks, I will be sharing a series of articles offering practical pearls from various lectures presented at ODAC 2018, along with original content. I am a 1st year Dermatology Resident at George Washington University School of Medicine and Health Sciences in Washington, DC. I truly love being in the greatest specialty in medicine. Every day is full of surprises, from a patient walking into your Mohs clinic with a 7cm periorbital tumor to an erythrodermic patient unable to stop shivering and wondering what has caused his condition. I’m so grateful that I get the chance to be involved in the care of these patients at multiple clinical sites. There’s no other field that allows you to merge aspects of Internal Medicine, Pediatrics, Surgery, Dermatopathology, Cosmetics, and more…all in one day. You truly never know what you’re going to get behind each door.
On this cheerful note, I would like to introduce part 1 of my first topic: “Practical Pearls in Cutaneous Fungal Infections and Onychomycosis” by Dr. Adam Friedman. As a 1st year dermatology resident, I have quickly realized that I need to be proficient in accurately diagnosing fungal infections. According to the National
Ambulatory Medical Care Survey (NAMCS) and National Hospital Ambulatory Medical Care Survey (NHAMCS), there is an estimated average of 4.1 million annual visits for dermatophytosis. So it’s true… fungus is among us!
When it comes to making the diagnosis, there are several options:
1. Potassium hydroxide (KOH) microscopy: detects hyphae and conidia in skin
scrapings or hair. This is 1st line!
a. It is important to take at least 2 samples for the KOH examination
when you clinically suspect tinea pedis, and 3 samples when there
are keratotic lesions.
b. Reminder: Will be negative for Majocchi’s granuloma.
2. Wood’s lamp examination: Detects fluorescence in some dermatophytes, including some strains of the zoophilic and anthropophilic dermatophytes.
3. Fungal cultures: required to identify the organism, but not as sensitive as KOH or histopath.
4. Skin biopsies or nail clippings: Periodic Acid Shift (PAS) will show live fungus, while GMS will show live and dead fungus.
Now, let’s briefly review some of the common infections, including their clinical presentations and the organisms responsible:
1. Tinea faciei
– CLINICAL: Seen on non-bearded parts of the face; pruritus or burning may worsen with sunlight exposure

– ORGANISM: T. tonsurans (N America), T. mentagrophytes and T. rubrum (Asia)
2. Tinea barba
– CLINICAL: Seen on unilateral neck/face; types include deep nodular suppurativa vs superficial crusted plaques with folliculitis
– ORGANISM: T. mentagrophytes, T. verrucosum
3. Tinea pedis
– ** Most common form of cutaneous fungal infection**
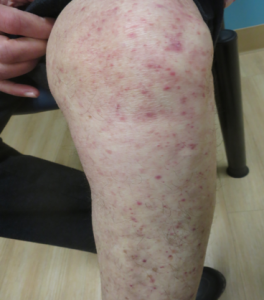
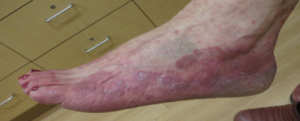
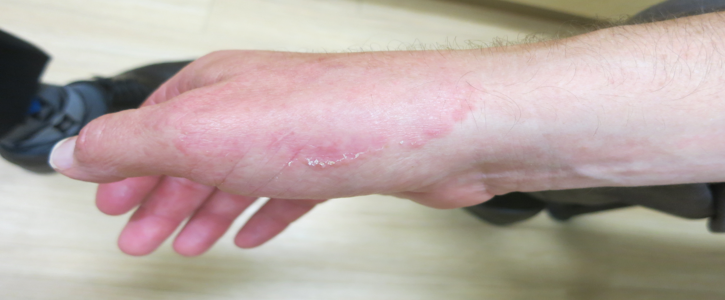
– 4 types: moccasin, interdigital, vesicular, ulcerative
a. Moccasin
Chronic and often resistant type characterized by fine, silvery scale with pink, tender and itchy skin
PEARL ALERT!!! **2 HANDS, 1 FOOT OR VICE VERSA**
T rubrum
b. Interdigital
Interweb infections often involve fungi, yeast, and bacteria
c. Vesicular
Inflammatory chronic fungal infection seen with use of occlusive footwear, presenting with vesicles or bullae on sole Be aware that you can get a dermatophytid reaction presenting with itchy sterile vesicles on fingers, chest and arms (allergic response)
T. mentagrophytes (KOH from roof of blister)
– ORGANISM: T. rubrum (most infections), T. mentagrophytes (bullous subtype)
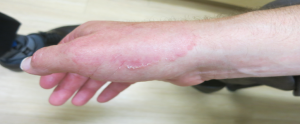
4. Tinea Manuum
– CLINICAL: Classic “ringworm” appearance on dorsal hand vs dry, scaly and keratotic lesions on palmar surface of hand; nails often affected
5. Tinea Cruris (aka “jock itch”)
– CLINICAL: Symmetric, annular red, scaly plaques with active border starting in the crural folds of the groin, most commonly seen in men > women
– PEARL ALERT!!! *IMPORTANT -> SPARES SCROTUM AND PENIS*
– ORGANISM: T. rubrum, T. mentagrophytes, E. floccosum
6. Tinea Capitis
– CLINICAL: Noninflammatory (black dot or seborrheic) vs Inflammatory (kerion) or combination of both variants; broken hairs are prominent feature – Kerion is a painful, boggy mass with broken hair follicles with higher risk of scarring.
PEARL ALERT!!! You should perform fungal AND bacterial culture!!! (scrape off scale using toothbrush then submit toothbrush, scale and fungal cotton-tipped applicator for culture)
+cervical, occipital or postauricular lymphadenopathy is common
– ORGANISM: T tonsurans (US), M canis (worldwide)
7. Tinea Incognito
– CLINICAL: Dermatophyte infection with an atypical presentation because of the use of topical steroids
That’s all for now. Be on the look out for my next article in which I’ll highlight the 2nd half of Dr. Friedman’s lecture focusing on onychomycosis and treatment of all of these fungal infections. Until then… IF IT’S SCALY, SCRAPE IT!!!
Images: courtesy of Dr. Adam Friedman
Next Steps Correspondent

Dr. Eleryan is a Dermatology Resident, PGY-2 at The George Washington University School of Medicine and Health Sciences. She received her undergraduate degree in Chemistry from North Carolina State University. She completed her Master of Science in Biomedical Sciences at Philadelphia College of Osteopathic Medicine. She continued her medical training at Ross University School of Medicine, where she graduated with High honors. Her interests include cutaneous t-cell lymphoma (CTCL), melanoma, and dermatologic surgery.