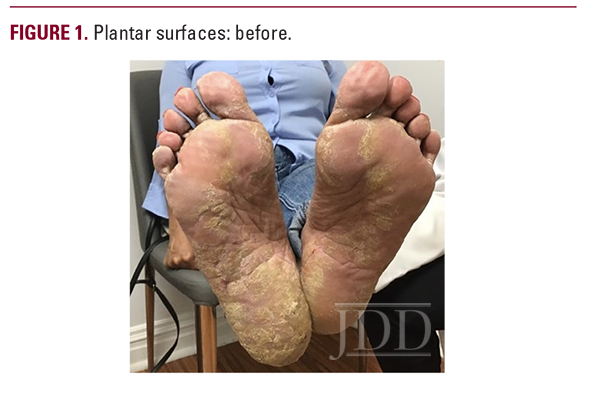
A 64-year-old female presented to the outpatient clinic for the evaluation of flaking and itchy lesions on her bilateral hands and feet that were present for several months and caused difficulty with activities of daily living. Inconsistent use of betamethasone and narrowband ultraviolet (UV)-B on the affected areas were both reported, neither of which improved the patient’s symptoms. The physical exam was remarkable for yellow plaques with moderate scaling on over 50% of the patient’s bilateral palmoplantar surfaces (see Figures 1, 3). The differential diagnosis included palmoplantar keratoderma, tinea pedis, and psoriasis. A fungal culture was performed from the patient’s right plantar foot, but ultimately came back negative for growth after one month. Upon follow up at the one-month mark, a shave biopsy was performed on the right plantar surface to rule out psoriasis vs palmoplantar keratoderma.

Histopathology revealed hyperkeratosis with neutrophils within mounds of parakeratosis, digitated and psoriasiform epidermal hyperplasia, dilated blood vessels at the tips of dermal papillae, and a superficial perivascular mixed inflammatory cell infiltrate. The condition was diagnosed as verrucous psoriasis (VP); since there is currently no standard treatment protocol for VP, the options of topical steroids, calcineurin inhibitors, vitamin D analogues, intralesional kenalog, and apremilast were considered. Ultimately, the decision to start apremilast was made; the patient started the 5-day titration schedule and went on to complete the 28 day starter pack.
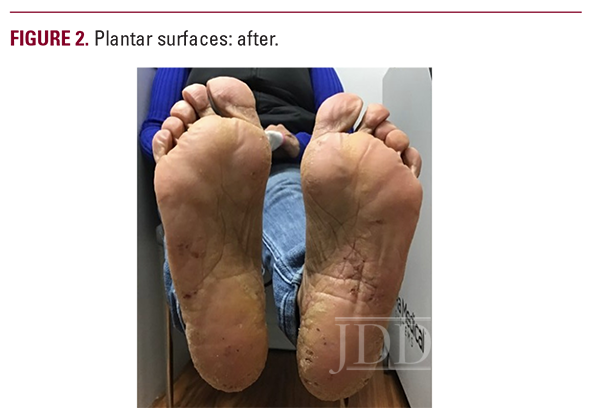
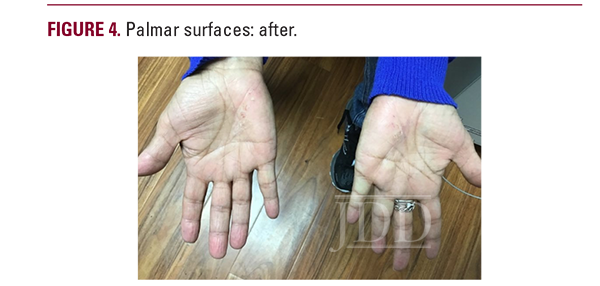
Upon completion of the starter pack, the patient returned to the clinic for re-evaluation, at which time she denied side effects of depression or headaches, but admitted to mild gastrointestinal (GI) upset that self-resolved. Upon exam, the patient’s lesions were reduced in size by approximately 50% on all surfaces and were lessened to mild in severity (Figures 2, 4). To our knowledge, this is the first time that apremilast has ever been used in the treatment of VP and we found that this novel approach significantly improved the patient’s quality of life.
COMMENTARY
We had marked success with a novel approach for treating the rare and poorly understood condition of verrucous psoriasis by using apremilast.2 In previous reports, patients were given kenalog and/or topical steroids with varying degrees of success.3-6 Although upwards of 3 million cases of psoriasis are diagnosed annually in the US, verrucous psoriasis has only 20 reports currently in the literature.1 Via this prototypical treatment with apremilast, we hope to shed some light on this otherwise not-well-understood and unusual histopathological variant of psoriasis.
DISCLOSURES
The authors have no conflicts of interest to declare.
REFERENCES
1. Khalil FK, Keehn CA, Saeed S, et al. Verrucous psoriasis: a distinctive clinicopathologic variant of psoriasis. Am J Dermatopathol. 2005;27(3):204-207. doi:10.1097/01.dad.0000157450.39033.31
2. Maloney NJ, Zhao J, Tegtmeyer K, et al. Off-label studies on apremilast in dermatology: a review. J Dermatolog Treat. 2020;31(2):131-140. doi:10.1080 /09546634.2019.1589641
3. Moesch J, Mercer J, Sissom J, et al. A rare case of verrucous psoriasis in young female: a case report and review of clinicohistologic presentation and variable therapeutic response. J Amer Osteopath Col Dermatol. 2016;34:56-58.
4. Monroe HR, Hillman JD, Chiu MW. A case of verrucous psoriasis. Dermatol Online J. 2011;17(5):10. doi:/10.5070/D30cn3d92h
5. Sergeyenko A, Clay T, Guo, AM. A case of verrucous psoriasis. J Dermatol Nurses Assoc. 2017;9(4):183-185. doi: 10.1097/JDN.0000000000000299.
6. Shivers L, Montanez-Wiscovich ME. Verrucous psoriasis treated with methotrexate and acitretin combination therapy. Cutis. 2019;104(6):E10-E12.