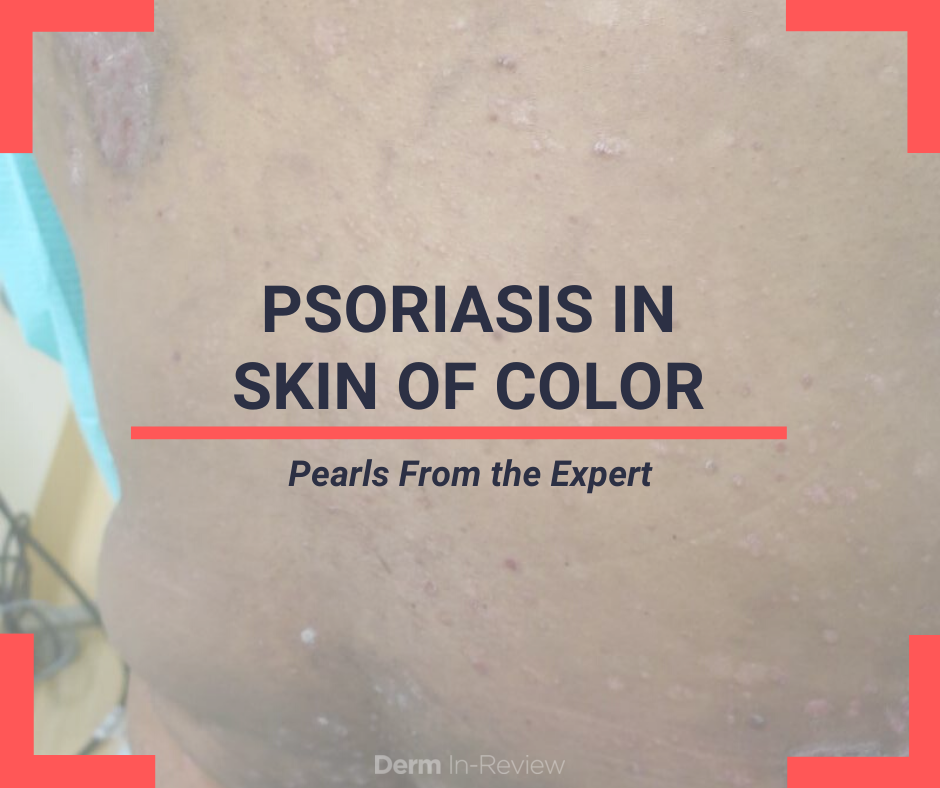
As a first-year dermatology resident, I really enjoyed Dr. Andrew Alexis’ lecture on Psoriasis: Distinct Clinical Features and Treatment Options for Psoriasis Patients of Color at the Skin of Color Update. His lecture largely focused on the fundamentals of dermatology. He emphasized the importance of looking at color and distribution of the clinical presentation and recognizing common mimickers of psoriasis such as lichen planus, sarcoidosis, and cutaneous lupus erythematosus (i.e. discoid lupus) in skin of color. Previously, psoriasis was thought to be rare in patients of African ancestry. However, even though Caucasians have the highest prevalence at 3.6%1, African Americans have a prevalence of 1.6%1 and Hispanics have a prevalence of 1.4%1. The classic presentation of psoriasis having a bright red plaque with silvery scale is not so classic in patients of African descent because of the lack of perceptible erythema. Instead, dermatologists must train their mind’s eyes for nuances in the clinical presentation and pay attention to shades of purple (violaceous hues), red-brown, and even gray presentations of psoriasis plaques. The location and distribution of the plaques on extensor surfaces and the sharply demarcated borders are also very helpful clinical clues for psoriasis. However, Dr. Alexis emphasized that when in doubt, do not hesitate to biopsy.
During the lecture, Dr. Alexis played a game of psoriasis or not with the audience where the audience by raising their hands would guess if the Kodachrome was psoriasis. This game illustrated the vast presentation of psoriasis and how papulosquamous disorders such as lichen planus can be challenging to differentiate from psoriasis. Another challenge of psoriasis in skin of color can be post-inflammatory pigment alteration and the impact of quality of life. The pigment alteration can be hyperpigmentation or hypopigmentation. Even after clearing the plaques of psoriasis, pigment alteration can last for weeks, months, or years. Considering the effects on pigment when deciding on the appropriate treatment regimen can be very helpful, such as counseling a patient that using phototherapy or excimer laser may lead to the treated areas getting darker.
In addition, Dr. Alexis highlighted a survey by the National Psoriasis Foundation that showed the greater psychosocial impact of psoriasis as well as more severe disease in African-Americans than Caucasians.2 Dr. Alexis discussed while systemic biologic treatments are safe and efficacious in patient populations from diverse backgrounds and data on specific non-white racial and ethnic groups are limited due to lower enrollment in psoriasis clinical trials.3
Lastly, Dr. Alexis discussed scalp psoriasis in women of African ancestry and how it is advantageous to discuss with the patient their hair care practices, including hair washing frequency and hairstyles. For topical treatments for scalp psoriasis in women of African descent, he prefers a combination of calcipotriene and betamethasone dipropionate that is in a vehicle of mineral oil and castor oil because it tends to be well tolerated in Afro-textured hair.4 However, he has a low threshold for using non-topical therapies such as systemic biologic agents including etanercept, adalimumab, and secukinumab. With psoriasis and scalp psoriasis, it is important to pay attention to the nuances of how the pathology may present in patients of skin of color and working with the patient on treatments that can help to avoid disfiguring pigmentary changes and treatments that are amenable to cultural practices such as hair care styling practices and frequency of hair washing.
References
- Rachakonda TD et al. Psoriasis prevalence among adults in the United States. J Am Acad Dermatol 2014;70:512
- National Psoriasis Foundation. Report on the psycho‐social impact of psoriasis. 2009. http://www.psoriasis.org/Document.Doc?id=619
- Alexis AF, Blackcloud P. J Clin Aesthet Dermatol. 2014;7(11):16
- Tyring S. et al. Int J Dermatol 2010, 49, 1328
Did you enjoy this article? Find more on Skin of Color here.
Next Steps in Derm is brought to you by SanovaWorks.