Sleep is essential for our overall well-being and one of the pillars of atopic dermatitis management. Unfortunately, we don’t learn or talk about this much in dermatology. Don’t fret- Dr. Vivian Shi shares her integrative strategies for optimizing sleep in atopic dermatitis!
Can you imagine what your life would be like if you weren’t able to sleep well for more than 5 nights a week? That’s what more than half of moderate-to-severe atopic dermatitis (AD) patients experience. In fact, over 60% of children with AD experience disturbed sleep patterns, which increases to 90% during flares. It’s no wonder they have higher risks of learning disabilities, cognitive delay, impulsivity, hyperactivity, and attention deficit. I would, too!
And for the family? Similar sleep deprivation, frustration, exhaustion, and reduced emotional well-being—for everyone. Sadly, it’s not uncommon for parents of severely affected children to reduce their work hours or quit work altogether to care for these children—further adding to the stress. Can we, as dermatologists, make this better?
Unfortunately, we don’t learn or talk about this much in dermatology. That’s why it was delightful and refreshing to hear Dr. Vivian Shi’s pearls on integrative strategies for optimizing sleep in atopic dermatitis, presented at the Integrative Dermatology Symposium 2019.
Let’s talk circadian rhythm
“Doc, I’m so itchy at night!” shares the suffering patient. “Well, it’s because all is quiet and you have nothing else to do at night but to think about your itchy skin (obviously),” you explain eloquently. How often does this conversation take place? For me, everyday— honestly. Until now.
Turns out– there are multiple physiologic reasons for increased itching night: increased transepidermal water loss, less oil production, hyperactive immune cells that work overtime to produce inflammatory cytokine production, and unstable blood vessels that lead to more histamine release.
Yes, the skin in fact has a tight diurnal pattern. “Circadian dosing” is utilized in other fields to maximize efficacy of certain medications. Why not for AD?
Pillars of AD treatment
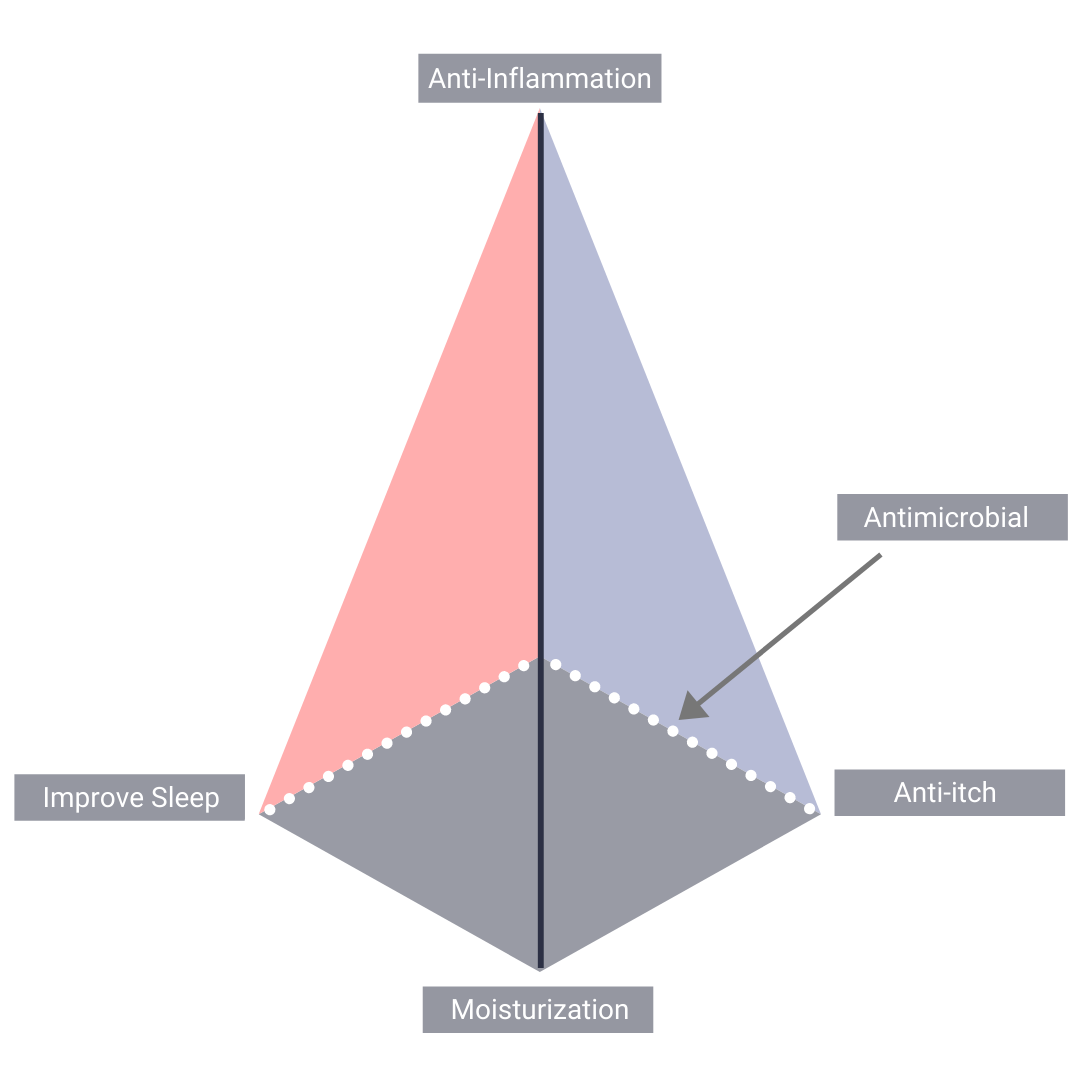
There are 5 pillars of treatment of AD:
1. anti-inflammation
2. improve sleep
3. antimicrobial
4. anti-itch
5. moisturization
Interestingly, of 14 guidelines for atopic dermatitis published thus far across the globe, there was surprisingly little to none addressing sleep, other than antihistamines – leaving a significant gap in care for AD patients.
Integrative strategies for sleep
Here are some practical tips that Dr. Shi shares for improved sleep. Instead of going to antihistamines as first-line, these are excellent tips to share with patients (and friends/family!) We could all use higher quality sleep, right?
-
Optimize the sleep environment
- Maintain cool ambient temperatures, as sweating is an irritant and makes itching worse
-
-
- Use a cooling mattress, such as the Purple® mattress, bamboo mattress topper or a gel mattress topper
- Limit the number of blankets used
-
-
- Change from blue light to warm ambient lighting, as blue light reduces melatonin production
-
-
- Change the setting on electronic devices
- Use blue light blocking glasses
-
-
- Use hypoallergenic fabrics for bed sheets, pillowcases, and blankets
- Use a HEPA filter to decrease dust mite and pollutants
-
Behavioral modification
- Regular aerobic exercise in the morning or afternoon (rather than the evening) — increases sleep quality
- Avoid co-sleeping, which can disrupt sleep quality for co-sleepers
- Avoid eating at least 3 hours before bedtime.Indigestion can interfere with sleep
- Avoid caffeine or nicotine (and other stimulants) at least 6 hours before bedtime
- Prior to bedtime, administer asthma and allergy medications to help breathe better
-
Massage therapy
- A study showed that children with AD who had a 20-min massage nightly for 1 month had lower anxiety, AD severity, and itch
- May work by increasing moisturizer penetration
- Caution: avoid aromatherapy with essential oils and olive oils that can disrupt the skin barrier (side tip: olive oil is not good for AD skin!)
- Use natural cold-pressed oils, such as virgin sunflower seed, coconut, and borage seed oil
-
Wet wraps have a cooling anti-itch effect, with or without medications!
-
- Step 1: soak wraps (thin cotton pajamas) in warm water
- Step 2: bathe or shower in warm water
- Step 3: after bathing, lightly pat dry with a towel
- Step 4: within 3 minutes, apply a moisturizer or a prescription medication on semi-dry skin
- Step 5: wring out excess water from the pajamas and put the damp pajamas it on
- Step 6: apply another dry layer of pajamas on top before bed
-
Music therapy
-
- Delta-waves have been shown to improve sleep and reduce AD severity
- Can be easily found on Youtube or apps
-
-
Acupuncture
- Works by increasing serotonin and GABA and reducing glutamate levels
- In a randomized controlled study (compared to sham points), acupuncture 3 times weekly for 4 weeks led to improvement in insomnia
-
Melatonin
- In a study, AD children who received melatonin 3mg daily had shortened sleep latency onset and improved disease, compared to controls
- Recommended dosing: 3-5 mg 30 to 60 minutes before desired sleep time
- Caution: melatonin can have possible hypothalamic-gonadal axis suppression with long-term use and can lower the seizures threshold (always ask about seizure history!)
When all else fails, antihistamines and other pharmaceutical rescues. Here are dosing recommendations:
-
-
- Diphenhydramine – 30 minutes before bedtime, as needed: > 12 years old: 25-50 mg; < 12 years old: 1-2mg/kg
-
-
-
- Hydroxyzine –30 minutes before bedtime, as needed: >12 years old: 25mg as needed; <12 years old: 0.5mg/kg before bedtime. Caution: some generic pills contain lactose
-
-
-
- Cyproheptadine (safe in pregnancy) – 30 minutes before bedtime, as needed: >12 years old: 4mg; <12 years old: 2-4mg
-
Caution with all antihistamines: tolerance can develop with long-term use; paradoxical excitation can occur.
-
-
- Mirtazapine (safe in pregnancy): Adults: 15mg nightly, titrated up to 45mg as needed. Children and elderly: 7.5mg nightly, titrate up to 15mg as needed
-
-
-
- Doxepine: Adults: 3-6mg nightly; Children: 1.5-3mg nightly
-
Some other fun ideas to reduce heat which can worsen nocturnal itch!
-
-
- Cooling pillow and eye masks
- DIY rice starch mask. Whatever you have left over, you can make spring rolls!
-
Lastly, there are free eczema ebooks available for free download on www.learnskin.com! Check them out, and also join the 2020 Integrative Dermatology Symposium in Sacramento!
Did you enjoy this article? Find more on Integrative Derm Topics here.
Next Steps in Derm is brought to you by SanovaWorks.

