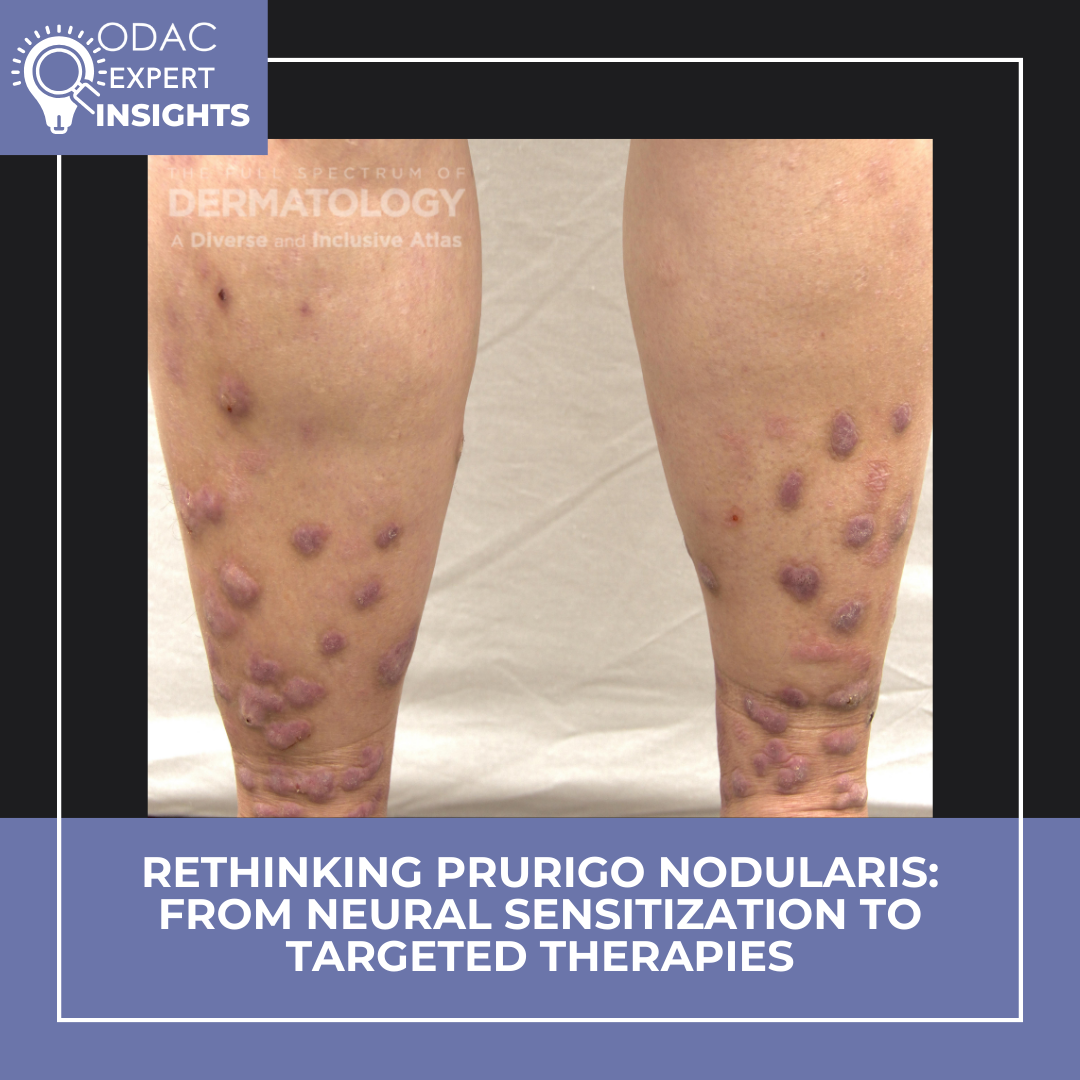
At the 2026 ODAC Dermatology conference, Dr. Adam Friedman opened his session on prurigo nodularis (PN) with a patient case that felt familiar to many of us. A patient with multiple nodules, relentless itch, and one central question. Why is this happening?
This patient case reminds us that prurigo nodularis is not simply the result of scratching or a sequela of another inflammatory disease. It is a distinct neuroinflammatory disorder with systemic implications. Dr. Friedman emphasizes that overlap does not mean sameness. With the advent of targeted therapies for PN, it is even more important that we distinguish prurigo nodularis from other potentially overlapping diagnoses.
The Diagnostic Gray Area
PN occupies a broad clinical spectrum and can mimic many dermatologic conditions. The core features are chronic pruritus lasting more than six weeks, repeated scratching, and hyperkeratotic nodules. The challenge is that these features are not exclusive to PN.
Atopic dermatitis, chronic kidney disease associated pruritus, psychogenic excoriation, and other inflammatory dermatoses can present with similar patterns. In clinic, the recurring question becomes whether this is habitual picking or something more.
While there is overlap, PN is not merely behavioral. The nodules we see are the physical imprint of a pathologic itch scratch cycle driven by immune and neural dysregulation. This distinction matters because if we mislabel it, we miss the mechanism.
A Neuroimmune Circuit, Not Just Inflamed Skin
Dr. Friedman emphasized that PN is sustained by a maladaptive neuroimmune loop. It carries T2 features, but it is not simply another version of atopic dermatitis.
IL-4 and IL-13 contribute to the inflammatory environment. However, IL-31 sits at the center of the itch axis. Produced by activated Th2 cells, IL-31 binds directly to receptors on cutaneous sensory neurons, signaling the nerves in real time and driving itch and scratching behaviors.
Periostin further amplifies this communication. Beyond its structural role in the extracellular matrix, periostin binds integrins on sensory neurons to enhance itch transmission while simultaneously stimulating keratinocytes to release additional inflammatory mediators. The result is a feed forward loop of inflammation heightening neural sensitivity, and neural signaling perpetuating the inflammation. Chronic scratching then reshapes the skin. Mechanical injury drives epidermal hyperplasia, dermal fibrosis, and increased nerve fiber density within lesional skin. Neural remodeling lowers the threshold for itch perception.
This framework supports the emerging concept of two clinical subtypes: 1) inflammatory predominant PN driven largely by cytokine signaling and 2) neuropathic predominant PN is sustained by neural sensitization. The distinction is clinically relevant as it may explain why some patients respond dramatically to targeted immune therapy while others require neuromodulation to quiet peripheral and central sensitization.
This distinction also clarifies why antihistamines often disappoint. Histamine is not the dominant mediator in PN, and sedation is not disease modification. We are not simply treating itch. We are trying to interrupt a circuit.
PN Rarely Travels Alone
Although PN is a distinct disease, it frequently co-exists with other systemic conditions. Atopic dermatitis, hepatitis C, chronic kidney disease, and congestive heart failure are commonly seen alongside it. Systemic inflammation and metabolic stress may lower the threshold for neural activation and immune dysregulation, reinforcing the neuroimmune loop.
Lifestyle factors such as smoking, obesity, alcohol use, and poor diet further compound this dysregulation. We must not forget the substantial cost burden of PN and profound impact on the quality of life of our patients. Sleep disruption, visible nodules, chronic discomfort, and stigma all converge. When Dr. Friedman returned to the initial patient case, it was a reminder that beyond the mechanistic pathways, this disease carries real human weight.
Where Do We Go from Here
Management of PN can be framed around three core goals.
-
- Reduce the itch.
- Interrupt the itch-scratch cycle.
- Heal the lesions.
Before discussing treatments, Dr. Friedman emphasizes that expectation setting is critical. Even with effective therapy, scars and dyspigmentation may persist. Control rather than cure remains the practical objective.
Therapeutically, treatment can be conceptualized across two domains: nerves and immunology.
Topical therapies still have a role in PN. Emerging data on topical ruxolitinib are encouraging, particularly in inflammatory predominant disease. Palmitoylethanolamide (PEA) enhances the endocannabinoid system and offers an adjunctive approach targeting neural modulation.
Neuromodulators remain essential tools. In a playful yet memorable slide titled Yo (GABA) GABA, Dr. Friedman highlighted gabapentin and pregabalin as foundational options when titrated slowly and thoughtfully. Mirtazapine at lower doses may improve nocturnal itch, though weight gain must be discussed openly with patients. Naltrexone may benefit select individuals at low doses. In patients with severe inflammatory flares, Intramuscular corticosteroids can be helpful and given in the office.
The biologic era has shifted the landscape. IL-31 blockade with nemolizumab aligns directly with mechanism and represents a significant advance. For some patients, monotherapy is sufficient; while for others, combination strategies will likely be necessary. JAK inhibition remains an exciting frontier, with agents such as povorcitinib under investigation and offering potential expansion of targeted options.
Once clear, how do we keep patients clear? Dr. Friedman kept the message simple. “Stay on to stay clear”, he emphasizes. Abrupt withdrawal often leads to recurrence. Maintenance strategies are essential for many patients, and as our therapeutic armamentarium grows, so does our ability to individualize long term management.
The Takeaway
Prurigo nodularis is increasingly recognized as a distinct neuroimmune disease with identifiable pathways and targeted treatments. The challenge moving forward is identifying which patients fit the inflammatory or neuropathic phenotype and when combination therapy is warranted.
As we continue to align mechanism with management, our goal remains fewer nodules, improved quality of life, and a durable treatment response. For patients who continue to ask why, we are finally getting closer to an answer that makes sense biologically and therapeutically.
This information was presented by Dr. Adam Friedman during the 2026 ODAC conference. The above highlights from her lecture were written and compiled by Dr. Tammy Gonzalez. Dr. Gonzalez was one of the five residents selected to participate in the Young Dermatology Leader Mentorship Program sponsored by Sun Pharma and organized by Derm In-Review.